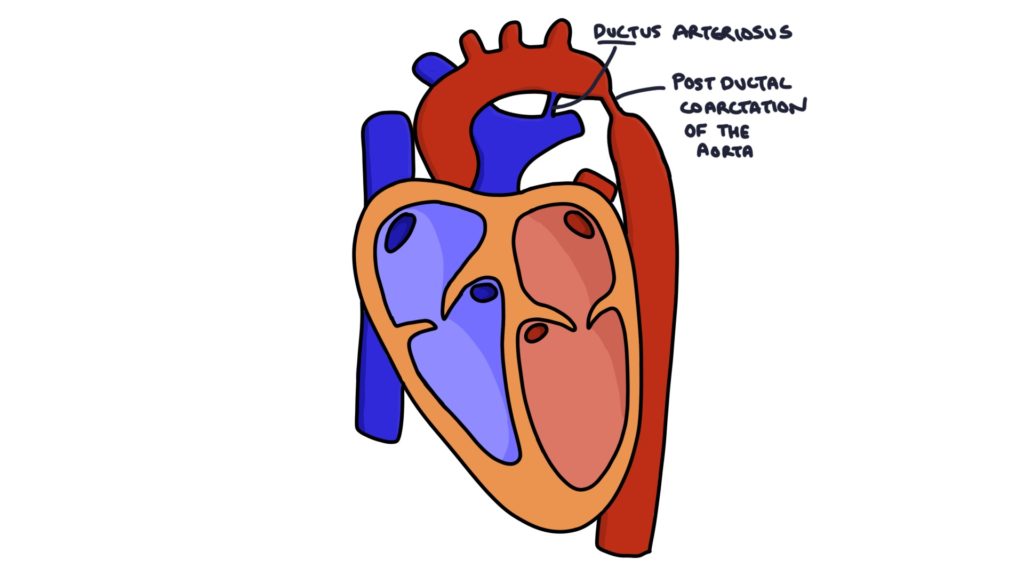
Coarctation of the aorta is a congenital condition involving a narrow point in the aortic arch, usually near the ductus arteriosus. The severity varies from mild to severe. It may be associated with a genetic condition, particularly Turner’s syndrome.
There is increased pressure proximal to the narrowing and decreased pressure distal to the narrowing.
Presentation
The only indication in a neonate may be weak femoral pulses (part of the routine newborn baby check).
Blood pressure readings from all four limbs show:
- Increased pressure in the limbs supplied by vessels proximal to the narrowing (e.g., arms)
- Reduced pressure in the limbs supplied by vessels distal to the narrowing (e.g., legs)
Coarctation can produce a systolic murmur heard below the left clavicle and left scapula.
Other signs in infancy (depending on the severity):
- Raised respiratory rate
- Increased work of breathing
- Poor feeding
- Heart failure
- Shock
Additional signs may develop over time:
- Left ventricular heave due to left ventricular hypertrophy
- Underdeveloped left arm where there is reduced flow to the left subclavian artery
- Underdevelopment of the legs
Management
Management depends on the severity. Mild cases may not require surgical intervention. Severe cases may require emergency surgery shortly after birth.
Last updated January 2025
Now, head over to members.zerotofinals.com and test your knowledge of this content. Testing yourself helps identify what you missed and strengthens your understanding and retention.

