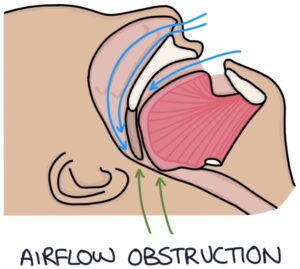
Obstructive sleep apnoea is caused by collapse of the pharyngeal airway. Apnoeas are episodes where the person stops breathing for up to a few minutes. Partners may report the episodes, while patients are often unaware of them.
Risk Factors
The risk factors for obstructive sleep apnoea are:
- Middle age
- Male
- Obesity
- Alcohol
- Smoking
Presentation
The presenting features of obstructive sleep apnoea are:
- Episodes of apnoea during sleep (reported by a partner)
- Snoring
- Morning headache
- Waking up unrefreshed from sleep
- Daytime sleepiness
- Concentration problems
- Reduced oxygen saturation during sleep
Severe cases can cause hypertension and heart failure and increase the risk of myocardial infarction and stroke.
TOM TIP: When suspecting obstructive sleep apnoea during a history, ask about daytime sleepiness and occupation. Daytime sleepiness should make you suspect obstructive sleep apnoea. Patients that need to be fully alert for work, such as heavy goods vehicle operators, require an urgent referral and may need amended work duties while awaiting assessment and treatment.
Epworth Sleepiness Scale
The Epworth Sleepiness Scale is used to assess symptoms of sleepiness associated with obstructive sleep apnoea.
Sleep Studies
Sleep studies are used to confirm the diagnosis, performed by an ENT or sleep specialist service.
A simple sleep study involves wearing an oxygen saturation monitor overnight at home.
Respiratory polygraphy involves wearing a more elaborate machine that monitors respiratory rate, flow rate (via a nasal sensor), saturations and heart rate, and can usually be done at home.
A complex sleep study involves an overnight stay in a sleep centre with polysomnography. It may include monitoring brain activity (EEG), muscle activity (EMG) and heart activity (ECG).
Management
Reversible risk factors should be addressed, with reduced alcohol, smoking cessation and weight loss.
Continuous positive airway pressure (CPAP) machines provide constant pressure to maintain airway patency.
Surgery is an option but involves significant surgical reconstruction of the soft palate and jaw. The most common procedure is called uvulopalatopharyngoplasty (UPPP).
Last updated June 2023
Now, head over to members.zerotofinals.com and test your knowledge of this content. Testing yourself helps identify what you missed and strengthens your understanding and retention.

