Parkinson’s disease is a condition where there is a progressive reduction in dopamine in the basal ganglia, leading to disorders of movement. The symptoms are characteristically asymmetrical, with one side of the body affected more. The typical patient is an older man, around 70 years old, with a gradual onset of symptoms.
There is a classic triad of features in Parkinson’s disease:
- Resting tremor (a tremor that is worse at rest)
- Rigidity (resisting passive movement)
- Bradykinesia (slowness of movement)
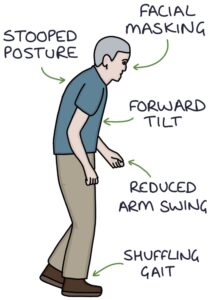
Pathophysiology
The basal ganglia are a group of structures situated near the centre of the brain. They are responsible for coordinating habitual movements such as walking, controlling voluntary movements and learning specific movement patterns.
Dopamine plays an essential role in the basal ganglia function. Patients with Parkinson’s disease have a slow but progressive drop in dopamine production.
Features
Tremor in Parkinsons is worse on one side and has a 4-6 hertz frequency, meaning it cycles 4-6 times per second. It is described as a “pill-rolling tremor” due to the appearance of rolling a pill between their fingertips and thumb. It is more noticeable when resting and improves on voluntary movement. It gets worse when the patient is distracted. Performing a task with the other hand (e.g., miming the act of painting a fence) exaggerates the tremor.
Rigidity is resistance to the passive movement of a joint. Taking a hand and passively flexing and extending the arm at the elbow demonstrates tension in the arm that gives way to movement in small increments (like little jerks). The jerking resistance to movement is described as “cogwheel” rigidity.
Bradykinesia describes the movements getting slower and smaller and presents in several ways:
- Handwriting gets smaller and smaller (micrographia)
- Small steps when walking (“shuffling” gait)
- Rapid frequency of steps to compensate for the small steps and avoid falling (“festinating” gait)
- Difficulty initiating movement (e.g., going from standing still to walking)
- Difficulty in turning around when standing and having to take lots of little steps to turn
- Reduced facial movements and facial expressions (hypomimia)
Other features include:
- Depression
- Sleep disturbance and insomnia
- Loss of the sense of smell (anosmia)
- Postural instability (increasing the risk of falls)
- Cognitive impairment and memory problems
TOM TIP: A common exam task challenges you to distinguish between the tremor of Parkinson’s disease and benign essential tremor. The table below gives some tips on this:
|
Parkinson’s Tremor |
Benign Essential Tremor |
|
Asymmetrical |
Symmetrical |
|
4-6 hertz |
6-12 hertz |
|
Worse at rest |
Improves at rest |
|
Improves with intentional movement |
Worse with intentional movement |
|
Other Parkinson’s features |
No other Parkinson’s features |
|
No change with alcohol |
Improves with alcohol |
Parkinson’s-Plus Syndromes
Multiple system atrophy is a rare condition where the neurones of various systems in the brain degenerate, including the basal ganglia. The degeneration of the basal ganglia leads to a Parkinson’s presentation. Degeneration in other areas leads to autonomic dysfunction (causing postural hypotension, constipation, abnormal sweating and sexual dysfunction) and cerebellar dysfunction (causing ataxia).
Dementia with Lewy bodies is a type of dementia associated with features of Parkinsonism. It causes a progressive cognitive decline. There are associated symptoms of visual hallucinations, delusions, REM sleep disorders and fluctuating consciousness.
Two other Parkinson’s-plus syndromes to be aware of are:
- Progressive supranuclear palsy
- Corticobasal degeneration
Diagnosis
Parkinson’s disease is diagnosed clinically based on the history and examination findings. The diagnosis should be made by an experienced specialist. The NICE guidelines (2017) recommend the UK Parkinson’s Disease Society Brain Bank Clinical Diagnostic Criteria.
Management
Treatment is initiated and guided by a specialist, tailored to each individual and their response to different medications. There is no cure. Treatment is focused on controlling symptoms and minimising side effects. Patients may describe themselves as “on” when the medications are acting, and they are moving freely, and “off” when the medications wear out, they are experiencing symptoms and their next dose is due.
The treatment options are:
- Levodopa (combined with peripheral decarboxylase inhibitors)
- COMT inhibitors
- Dopamine agonists
- Monoamine oxidase-B inhibitors
Levodopa is synthetic dopamine taken orally. It is usually combined with a peripheral decarboxylase inhibitor (e.g., carbidopa and benserazide), which stops it from being metabolised in the body before it reaches the brain. Levodopa is the most effective treatment for symptoms but becomes less effective over time. It is often reserved for when other treatments are not controlling symptoms.
Combination drugs are:
- Co-beneldopa (levodopa and benserazide), with the trade name Madopa
- Co-careldopa (levodopa and carbidopa), with the trade name Sinemet
The main side effect of levodopa is dyskinesia. Dyskinesia refers to abnormal movements associated with excessive motor activity. Examples are:
- Dystonia (where excessive muscle contraction leads to abnormal postures or exaggerated movements)
- Chorea (abnormal involuntary movements that can be jerking and random)
- Athetosis (involuntary twisting or writhing movements, usually in the fingers, hands or feet)
Amantadine is a glutamate antagonist that may be used to manage dyskinesia associated with levodopa.
COMT Inhibitors (e.g., entacapone) are inhibitors of catechol-o-methyltransferase (COMT). The COMT enzyme metabolises levodopa in both the body and brain. Entacapone is taken with levodopa (and a decarboxylase inhibitor) to slow the breakdown of the levodopa in the brain. It extends the effective duration of the levodopa.
Dopamine agonists mimic the action of dopamine in the basal ganglia, stimulating the dopamine receptors. They are less effective than levodopa in reducing symptoms. They are typically used to delay the use of levodopa, then used in combination with levodopa to reduce the required dose. Pulmonary fibrosis is a notable side effect with prolonged use. Examples are:
- Pramipexole
- Bromocriptine
- Pergolide
- Cabergoline
Monoamine oxidase-B inhibitors block the action of monoamine oxidase-B enzymes, helping to increase the circulating dopamine. Monoamine oxidase enzymes break down neurotransmitters such as dopamine, serotonin and adrenaline. Monoamine oxidase-B is more specific to dopamine. They are typically used to delay the use of levodopa, then in combination with levodopa to reduce the “end of dose” worsening of symptoms. Examples are:
- Selegiline
- Rasagiline
Last updated September 2023
Now, head over to members.zerotofinals.com and test your knowledge of this content. Testing yourself helps identify what you missed and strengthens your understanding and retention.

