Guillain-Barré syndrome is an acute paralytic polyneuropathy that affects the peripheral nervous system. It causes acute, symmetrical, ascending weakness and can also cause sensory symptoms. It is usually triggered by an infection and is particularly associated with to Campylobacter jejuni, cytomegalovirus (CMV) and Epstein-Barr virus (EBV).
Pathophysiology
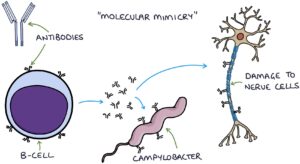
Guillain-Barré is thought to occur due to a process called molecular mimicry. The B cells of the immune system create antibodies against the antigens on the triggering pathogen. These antibodies also match proteins on the peripheral neurones. They may target proteins on the myelin sheath or the nerve axon itself.
Presentation
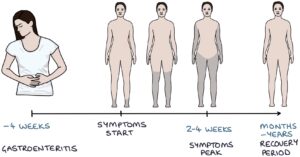
Symptoms usually start within four weeks of the triggering infection. They begin in the feet and progress upward. Symptoms peak within 2-4 weeks. Then, there is a recovery period that can last months to years.
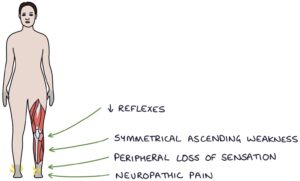
The characteristic features are:
- Symmetrical ascending weakness
- Reduced reflexes
There may be peripheral loss of sensation or neuropathic pain. It may progress to the cranial nerves and cause facial weakness. Autonomic dysfunction can lead to urinary retention, ileus or heart arrhythmias.
Diagnosis
The diagnosis of Guillain-Barré syndrome is made clinically (using the Brighton criteria), supported by investigations:
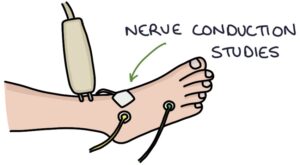
- Nerve conduction studies (showing reduced signal through the nerves)
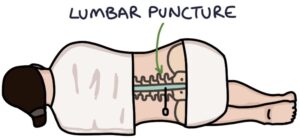
- Lumbar puncture for cerebrospinal fluid (showing raised protein with a normal cell count and glucose)
Management
Management involves:
- Supportive care
- VTE prophylaxis (pulmonary embolism is a leading cause of death)
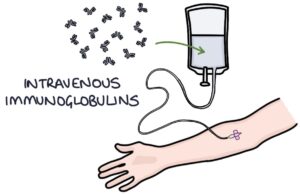
- IV immunoglobulins (IVIG) first-line
- Plasmapheresis is an alternative to IVIG
Severe cases with respiratory failure may require intubation, ventilation and admission to the intensive care unit.
Prognosis
Recovery can take months to years. Patients can continue regaining function five years after the acute illness. Most patients eventually make either a full recovery or are left with minor symptoms. Some are left with significant disability. Mortality is around 5%, mainly due to respiratory or cardiovascular complications.
Last updated October 2023
Now, head over to members.zerotofinals.com and test your knowledge of this content. Testing yourself helps identify what you missed and strengthens your understanding and retention.

