Antibiotics are used to treat infections caused by bacteria. They work in various ways to either stop the reproduction and growth of bacteria (bacteriostatic) or kill the bacteria directly (bactericidal). Over-use or inappropriate use can lead to antibiotic resistance and limited treatment options for infections.
Local Resistance and Guidelines
The bacteria in different populations develop resistance to different antibiotics. For example, the E. coli in one area of the country might be particularly resistant to trimethoprim, while another area has low levels of trimethoprim resistance. Therefore, it is necessary to have local policies that guide what antibiotics to use in different scenarios.
TOM TIP: In your OSCEs, questions about treating infections can be answered with “antibiotics according to the local antibiotic policy”, even if you have no idea what the usual choice would be.
Antibiotics That Inhibit Cell Wall Synthesis
Antibiotics with a beta-lactam ring:
- Penicillin
- Carbapenems such as meropenem
- Cephalosporins
Antibiotics without a beta-lactam ring:
- Vancomycin
- Teicoplanin
Antibiotics That Inhibit Folic Acid Metabolism
Bacteria produce folic acid in a series of steps. Para-aminobenzoic acid (PABA) is directly absorbed across the cell membrane into the cell. PABA is then converted to dihydrofolic acid (DHFA), then tetrahydrofolic acid (THFA), then folic acid.
Antibiotics can be used to disrupt steps along this chain:
- Sulfamethoxazole blocks the conversion of PABA to DHFA
- Trimethoprim blocks the conversion of DHFA to THFA
Co-trimoxazole is a combination of sulfamethoxazole and trimethoprim. Trimethoprim is bacteriostatic, while co-trimoxazole is bactericidal.
Metronidazole
Metronidazole is reduced into its active form in anaerobic bacteria. When partially reduced, metronidazole inhibits DNA synthesis. Metronidazole is very effective against anaerobes but not aerobes. It is bactericidal.
Antibiotics That Target Ribosomes
Antibiotics that inhibit protein synthesis by targeting ribosomes include:
- Macrolides (e.g., erythromycin, clarithromycin and azithromycin)
- Clindamycin
- Tetracyclines (e.g., doxycycline)
- Gentamicin
- Chloramphenicol
Nitrofurantoin
Nitrofurantoin is used exclusively to treat lower urinary tract infections. After being absorbed, it is present in very low levels in the blood and gets excreted and concentrated in the urine. Nitrofurantoin in the urine is absorbed into the bacteria cell, where flavoproteins reduce it into a highly reactive form, which attacks the bacterial DNA, ribosomes and other cell components.
It is bactericidal, meaning it directly kills the bacteria. It is not used to treat upper urinary tract infections (e.g., pyelonephritis) or infections in other areas, as it only achieves adequate concentrations in the urine and not the blood.
Penicillin Allergy
“Penicillin allergy” is very common. True penicillin allergy can lead to anaphylaxis and death and should not be taken lightly. However, true penicillin allergy accounts for around 10% of reported penicillin allergy. Being labelled as “penicillin allergic” stops patients from getting potentially life-saving antibiotics.
A small proportion of patients with a penicillin allergy will have a cross-reaction to cephalosporins and carbapenems. Cross-reactivity is often quoted at around 10% but is closer to 1% in reality.
TOM TIP: Always ask about the reaction when taking an allergy history. Diarrhoea, for example, is a side effect rather than an allergy and means, if necessary (e.g., in life-threatening sepsis), it can still be used.
Antibiotic Coverage
Use this table to think about how you could treat different presentations of patients with infections. For example, think about what antibiotics would be appropriate for a patient with a chest infection and why. This table is not exactly accurate and should not be used for treating patients but is helpful to gain an understanding of the general patterns.
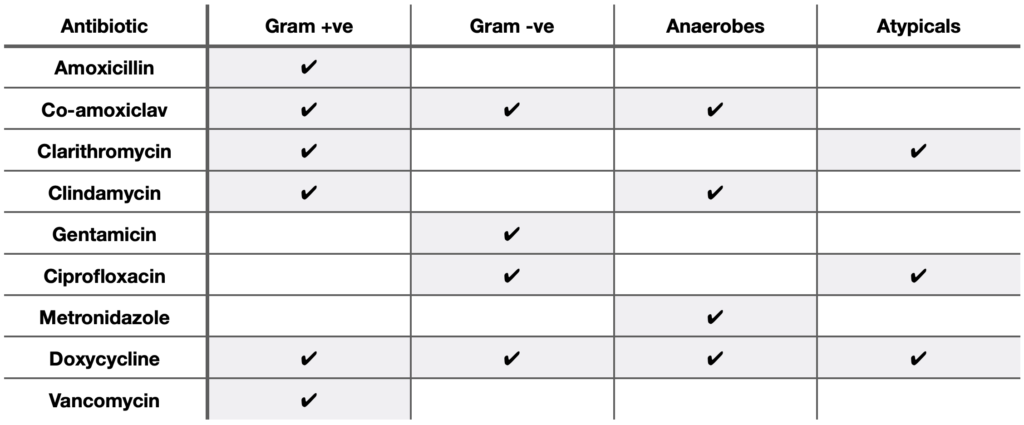
TOM TIP: When learning antibiotic coverage, I used this stepwise process of escalating antibiotic treatment in a hospital patient to remember what antibiotics covered what bacteria. Each step covers all the bacteria in the previous step as well as new ones:
- Start with amoxicillin which covers Streptococci, Listeria and Enterococci
- Switch to co-amoxiclav to additionally cover Staphylococci, Haemophilus and E. coli
- Switch to piperacillin with tazobactam (tazocin) to additionally cover Pseudomonas
- Switch to meropenem to additionally cover ESBLs
- Add teicoplanin or vancomycin to cover MRSA
- Add clarithromycin or doxycycline to cover atypical bacteria
Last updated July 2023
Now, head over to members.zerotofinals.com and test your knowledge of this content. Testing yourself helps identify what you missed and strengthens your understanding and retention.

