Malaria is an infectious disease caused by members of the Plasmodium family of protozoan parasites. Protozoa are single-celled organisms. The most severe and dangerous type is Plasmodium falciparum, which accounts for about 80% of malaria cases in the UK.
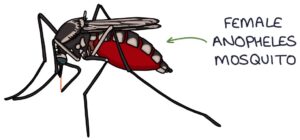
Malaria is spread through bites from the female Anopheles mosquitoes that carry the disease. Malaria is not transmitted in the UK and is associated with travel to areas where malaria is present.
Types
- Plasmodium falciparum (the most common and severe form)
- Plasmodium vivax
- Plasmodium ovale
- Plasmodium malariae
- Plasmodium knowlesi
Life Cycle
Malaria is spread by female Anopheles mosquitoes, usually at night. A feeding mosquito sucks up infected blood. Then, the parasites reproduce in the mosquito’s gut, producing thousands of sporozoites (malaria spores).
When that mosquito bites someone, the sporozoites are injected. These sporozoites travel to the liver of the newly infected person. P. vivax and P. ovale can lie dormant as hypnozoites for months or years before reactivating.
The malaria parasites mature in the liver into merozoites, which enter the blood and infect red blood cells. In red blood cells, the merozoites reproduce, after which the red blood cells rupture, releasing loads more merozoites into the blood and causing haemolytic anaemia.
For P. vivax and P. ovale, this rupture and release of merozoites occurs every 48 hours, causing a fever spike every other day. A fever every 48 hours is referred to as tertian malaria. P. falciparum has more frequent (“subtertian“) or irregular fever spikes, and P. malariae has spikes every 72 hours (“quartan“).
Presentation
Malaria should be suspected in someone that has travelled to an area where malaria is present. The incubation period is usually 1-4 weeks after exposure, although it can lie dormant for years.
Many of the symptoms are non-specific:
- Fever (up to 41ºC) with sweats and rigors
- Fatigue
- Myalgia (muscle aches and pain)
- Headache
- Nausea
- Vomiting
Signs on examination include:
- Pallor due to the anaemia
- Hepatosplenomegaly
- Jaundice (bilirubin is released during the rupture of red blood cells)
TOM TIP: The most characteristic symptom of malaria is the fever, which spikes very high every 48 hours. In someone with an unexplained fever, consider whether they have travelled somewhere with malaria present. Even exposure several years ago may be relevant, as P. vivax and P. ovale can lie dormant for up to 4 years.
Diagnosis
The diagnosis is made using a malaria blood film. This is sent in an EDTA bottle (the same bottle used for a full blood count). A malaria blood film will show the parasites, the concentration (as a percentage) and the type.
Three negative samples taken over three consecutive days are required to exclude malaria due to the parasites being released from red blood cells into the blood every 48-72 hours. The sample may be negative when the parasites are not released but positive a day or two later when the red blood cells rupture and release the parasites.
Management
The local infectious diseases team will advise on management. All patients with falciparum malaria are admitted.
Oral options for uncomplicated malaria include:
- Artemether with lumefantrine (Riamet) is the usual first choice
- Quinine plus doxycycline
- Quinine plus clindamycin
- Proguanil with atovaquone (Malarone)
- Chloroquine (there are increasing rates of resistance to chloroquine)
- Primaquine (can cause severe haemolysis in patients with G6PD deficiency)
Severe or complicated malaria often requires admission to HDU or ICU. Intravenous treatment options include:
- Artesunate is the usual first choice (haemolysis is a common side effect)
- Quinine dihydrochloride
TOM TIP: Remember artesunate and quinine as treatment options for your exams, as these are the most likely to be relevant. Remember that Plasmodium falciparum is the most common and severe cause, and these patients should be admitted for artesunate treatment and monitoring for complications.
Complications
There is a long list of complications of P. falciparum malaria, including:
- Cerebral malaria
- Seizures
- Reduced consciousness
- Acute kidney injury
- Pulmonary oedema
- Disseminated intravascular coagulopathy (DIC)
- Severe haemolytic anaemia
- Multi-organ failure and death
Prophylaxis
General advice for preventing malaria when travelling to endemic areas:
- No method is 100% effective alone
- Use mosquito spray (e.g., 50% DEET spray)
- Use mosquito nets and barriers in sleeping areas
- Seek medical advice if symptoms develop
- Take antimalarial medication as recommended
Antimalarial medications are not 100% effective. The main options are:
- Proguanil with atovaquone (Malarone)
- Doxycycline
- Mefloquine (risk of psychiatric side effects)
- Chloroquine with proguanil (less often used due to high resistance)
Proguanil / atovaquone (Malarone) is slightly more expensive than the other options but has the least side effects. It is taken from two days before until seven days after travel to an endemic area.
Doxycycline is a broad-spectrum antibiotic that can cause side effects such as diarrhoea and thrush. It also causes skin sensitivity to sunlight, increasing the risk of sunburn and skin reactions. It is taken two days before until four weeks after travel to an endemic area.
Mefloquine is associated with psychiatric side effects, such as anxiety, depression and abnormal dreams. Rarely it can cause psychosis or seizures. It is taken weekly, from two weeks before until four weeks after travel to an endemic area.
Last updated August 2023
Now, head over to members.zerotofinals.com and test your knowledge of this content. Testing yourself helps identify what you missed and strengthens your understanding and retention.

